Heart failure is a chronic condition in which the heart cannot pump blood as effectively as it should. While many people live with heart failure for years through proper treatment and lifestyle management, the condition can sometimes worsen. Recognizing early warning signs is critical. Prompt medical attention can prevent serious complications, hospitalization, or life-threatening events.
Understanding how heart failure progresses — and knowing what symptoms to watch for — empowers patients and caregivers to act quickly and protect heart health.
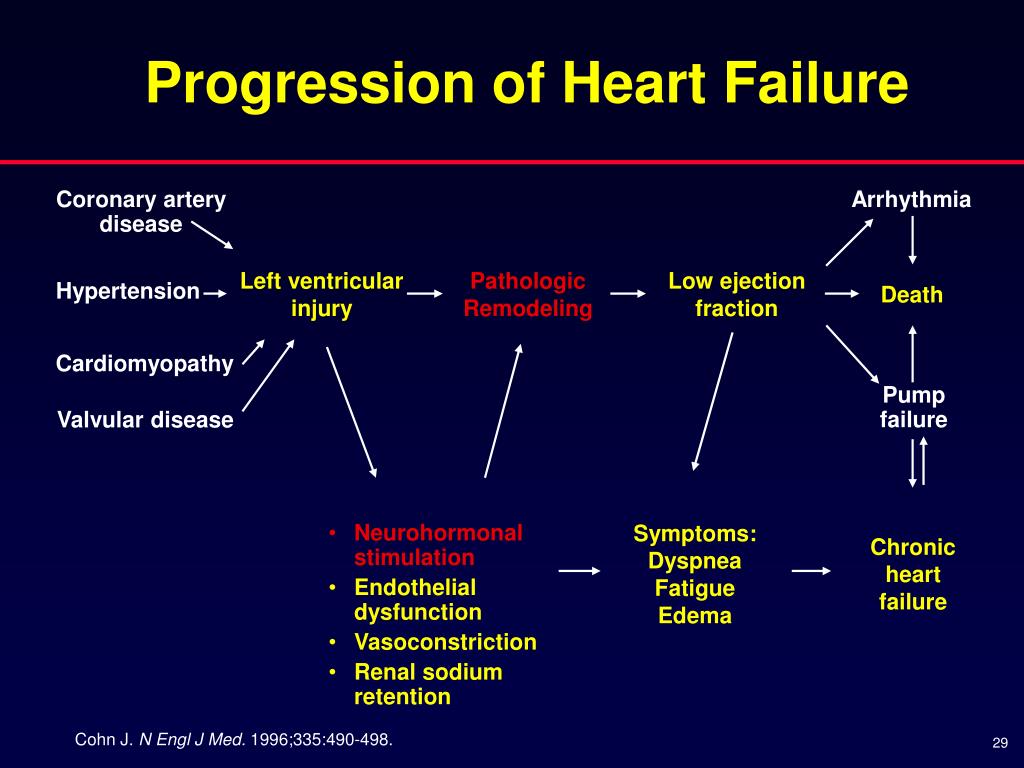
Heart failure does not mean the heart has stopped working. It means the heart’s pumping ability is weaker or stiffer than normal. Over time, the heart may struggle more to circulate blood efficiently, leading to fluid buildup and reduced oxygen delivery to the body.
Worsening heart failure may happen gradually or suddenly. Changes can occur due to medication issues, infections, dietary changes (especially excess salt), kidney problems, uncontrolled blood pressure, or another heart event.
Monitoring symptoms daily is essential for early detection.
One of the most common signs that heart failure is worsening is increased difficulty breathing.
You may notice:
As heart function declines, fluid can accumulate in the lungs, making breathing harder. If breathlessness becomes more frequent or severe, it requires immediate medical evaluation.
Rapid weight gain is often one of the earliest signs of fluid retention.
A gain of:
may indicate worsening heart failure.
This weight gain is not from fat but from fluid buildup in the body. Patients with heart failure are often advised to weigh themselves daily at the same time each morning. Sudden increases should be reported to a healthcare provider.
Fluid retention may cause noticeable swelling (edema), especially in:
Shoes may feel tighter, socks may leave deeper marks, and rings may become difficult to remove. Abdominal swelling can also cause discomfort or a feeling of fullness.
If swelling becomes more pronounced or spreads, it may indicate the heart is struggling to keep up with circulation demands.
A chronic cough that produces white or pink-tinged mucus can signal fluid buildup in the lungs. Wheezing may also occur.
This symptom is sometimes mistaken for a respiratory infection, but in heart failure patients, it can be a warning sign of worsening congestion.
If coughing increases or breathing becomes noisy and labored, medical assessment is necessary.

As heart function declines, less oxygen-rich blood reaches muscles and organs. This can lead to:
If everyday tasks such as walking across a room or climbing a few steps suddenly feel exhausting, this could signal worsening heart failure.
Persistent fatigue should never be ignored.
Fluid buildup in the abdomen can affect the digestive system. Some people may experience:
These symptoms may not immediately seem heart-related, but they can be linked to congestion and poor circulation affecting the liver and digestive tract.
When the heart weakens, it may try to compensate by beating faster.
You may notice:
Persistent or worsening palpitations can indicate arrhythmias, which are common in advanced heart failure and may require urgent treatment.
Reduced blood flow to the brain can cause:
Family members often notice these changes before the patient does. Sudden mental changes should be treated as a medical concern, especially in older adults.
Worsening heart failure can affect kidney function. This may result in:
Any significant change in urination patterns should be discussed with a healthcare provider.
While chest pain is more commonly associated with heart attacks, it can occur in people with heart failure, especially if coronary artery disease is present.
Chest pain, pressure, or tightness — especially when accompanied by shortness of breath, sweating, or nausea — requires immediate emergency care.
Call emergency services immediately if you experience:
These symptoms can signal a life-threatening complication.
Patients with heart failure are often advised to:
Even small changes can indicate worsening heart function. Early intervention often prevents hospitalization and serious complications.
Routine check-ups allow healthcare providers to adjust medications, monitor heart function, and identify issues early. Never stop or change heart medications without medical guidance, even if you feel better.
Lifestyle factors such as limiting salt intake, staying physically active within safe limits, avoiding smoking, and managing stress also play an important role in preventing progression.
Heart failure can worsen gradually or suddenly, but the body often gives warning signs. Increasing shortness of breath, sudden weight gain, swelling, fatigue, persistent cough, confusion, and changes in heart rhythm are all signals that should not be ignored.
Recognizing these symptoms early and seeking prompt medical care can make a significant difference in outcomes. If you or a loved one is living with heart failure, staying alert to changes and maintaining open communication with healthcare providers is essential for managing the condition safely and effectively.